
By the time you read this, around two billion people will be in some kind of COVID-19 lockdown.
For some, this will be merely an exercise in patience and finding ever more inventive ways of relieving boredom.
For others, it will be incredibly stressful.
There’s a lot around just now about dealing with COVID-related stress. Hopefully this provides a slightly different and useful angle for now and later.
COVID stress is real and legitimate
People are worried about getting sick, or their elderly parents or grandparents getting sick, afraid of losing their job or their business, worried about staff they may have, fearful of losing their house, fearful of tenancy problems, anxious about relationship dynamics, anxious about looming and possibly inevitable financial problems, worried about what they would do if something else happened on top of all this.
And people will lose jobs, they will lose businesses, and they will lose loved ones. They’re real and justified fears and, despite the differing nature of them, some things about stress are remarkably similar.
Your stress system helps identify things and assess them as threats, be that immediate or not, and real or potential. These threats are stressors. Your physical and emotional response, is stress.
For any event though, the brain looks to respond proportionally. The magnitude of the response should equal the magnitude of the event. Naturally, your response depends on the nature of the event, the context of the event, and the memories you have of events like it. By that we mean the nervous system ‘memory’ and your usual memories.
We all have an immediate response, and in the main it functions the same in everyone. It’s called SAM.
SAM. Your first responder
It comprises the Sympathetic nervous system, and the Adrenal Medulla. It’s shortened to some variation of the Sympatho-Adrenal Medullary axis.
It’s impressive. Here’s how it works.
Your triangular adrenal glands sit atop your kidneys, comprising a central component called the medulla, and an outer component called the cortex, each of which do different jobs. The medulla is responsible for releasing adrenaline and noradrenaline (also called epinephrine and norepinephrine) into your bloodstream.
These are necessary chemicals in your stress arsenal, and are from the catecholamine family.
The sympathetic nervous system is part of your autonomic nervous system – autonomic meaning it runs by itself without your input. The sympathetic system increases respiration, halts digestion and excretion, increases sweating and connects directly to your heart, allowing it to increase your heart rate and blood pressure. Adrenaline and noradrenaline from the adrenal medulla both amplify and prolong these effects.
This immediate, first responder system, then, is fast and short-acting, promoting rapid physiological change to facilitate extra alertness and awareness, so that you can decide how best to respond if you need to do so immediately. It’s a sprinter, a grunt up front approach, designed to give you what you need in the event of having to act immediately.
But there are considerations.
Implications of SAM
As a system, it learns over time what’s relevant for you, becoming more in tune with how you react and understand things. Because it’s largely out of your control, being autonomous, it does what it does whether you like it or not.
At present, it’s very likely that many people are awash with adrenaline, which lasts up to an hour in your system. While we have adrenaline, we also have increased cardiovascular activity and we’re generally on higher alert. One implication is that sustained increases in adrenaline are related to an increased risk of heart attack.
The more stressors you experience, the more active it is and the more sensitive it becomes. In addition to your heart rate being elevated more frequently, and your respiration, an over-sensitised SAM eventually leads to an over-response.
This can explain the sometimes out of character behaviour we see when we get to the ‘last straw’ and we behave in ways we ordinarily might not. If stress piles on stress, it’s no wonder we might not be the best version of ourselves.
Being in lockdown is a good time to understand how you, and others, might react, now that you know how SAM works. Remember, SAM sits largely outside conscious control.
Under the circumstances, maybe it isn’t entirely their fault.
Maybe we want to cut each other some slack.
COVID needs a different response
COVID-19 though, is not an immediate, as in the next two minutes, kind of threat. Unless you’ve been exposed, it’s a much more psychological threat. Might you lose your job? Might you lose your home? Might tension be high at home? Might you run out of food? Might you or a loved one catch it?
Even allowing for the pandemic modelling we have, what’s particularly problematic is that we’re not really sure what will happen, how bad things may get, if and in what way we’ll be personally affected and, especially, when it will end.
These things are difficult because the human brain’s default setting is to be afraid of the unknown.
Collectively, then, this is a substantially different set of demands on you, and they require a different set of responses, both physical and cognitive. Many of them are anticipatory, potential threats. They are long term and sustained, uncertain in magnitude, relentless even.
SAM won’t help. It simply isn’t built for prolonged stress. It’s a sprinter.
(By the way, the same mechanisms we’ll talk about next apply to situations of prolonged stress in different contexts, such as a bullying colleague or school mate, witnessing ongoing parental conflict, sustained financial stress, domestic abuse and so on.)
You need a marathoner. You need your HPA.
HPA. Your second responder
When you’re faced with a threat like these, your hypothalamus kicks into gear. It’s a complex bit of machinery, and it’s the H in HPA axis. The P stands for Pituitary and the A for Adrenal. The Hypothalamic Pituitary Adrenal axis.
Compared to SAM, the HPA is a slow burn. It may start at the same time but it needs the sustained pressure to perform.
A section of the hypothalamus releases three key chemicals in response to the threat. We’ll deal only with one, called CRH, or corticotrophin releasing hormone.
When CRH reaches your pituitary, also called the master gland for its control of hormones, it stimulates the corticotrophs to release yet another chemical in this cascade, called ACTH or adrenocorticotrophin hormone.
By now you know what adreno means.
ACTH acts on your adrenal glands but, unlike SAM which directs the inner medulla, ACTH acts on the outer section, the adrenal cortex.
Whereas adrenaline and its ilk are catecholamines, the adrenal cortex produces glucocorticoids, which are steroids. Chief among them in humans is cortisol. Cortisol then acts back on the pituitary, closing the loop.
Because glucocorticoids like cortisol are released into the bloodstream, they have virtually unhindered access to every cell you possess, resulting in widespread impact. Cortisol is extremely good at what it does, when stress is shorter term. When it’s more prolonged, cortisol can create some less favourable situations.
We’ll look briefly at only three.
Cortisol and weight
First, as a general rule of thumb, increased cortisol, along with stress, promotes weight gain.
Cortisol helps manage both our eating behavior and eating choices. It stimulates our inclination to eat, but not just for food as fuel. Cortisol stimulates our appetite for tasty, rich, fat and sugar dense food, better known as comfort food. When we’re stressed, we eat, and sometimes binge eat. That’s cortisol.
And it’s tricky because we eat comfort food to feel better, and less stressed. In other words, we eat comfort food to regulate our HPA axis. We eat to reduce stress, and it’s the stress which produces cortisol, which nudges, or even pushes, us, to eat junk.
And we gain weight.
Cortisol and sleep
Second, cortisol directly affects how well we sleep.
In a nasty little feedback loop, the adrenal cortex releases cortisol, which impairs our ability to sleep. When we lack sleep, the brain produces cortisol in response, which impairs our sleep, which results in more cortisol, which impairs our sleep. Worse, when we’re tired we tend to make poorer choices, including with food.
It’s absolutely a vicious circle.
Cortisol and memory
Third, is that cortisol plays with your memory.
The key memory structure in your brain is your hippocampus. It’s what converts short term memories into long term memories. You’d struggle without it.
It’s also highly sensitive to cortisol, due to the abundance of cortisol receptors it has. Unfortunately, the more cortisol you produce, the more receptors it fills and, the more receptors may be created for cortisol to fill. The problem is that cortisol destroys hippocampal brain cells.
With prolonged stress, and increased cortisol, there are measureable structural differences in your hippocampus.
It shrinks.
Lower hippocampal volume means impaired memory, particularly for declarative memory. The hippocampus and the HPA are linked, but with increased stress and some HPA dysregulation, the hippocampus suffers.
Putting them together
Together, these create significant disruption.
With COVID then, and many of us anticipating what may happen, people may be suffering regular short term increases in adrenaline, along with longer term increases in cortisol.
Our sympathetic nervous systems are running warm all the time, keeping our heart rate a bit higher, and our breathing a bit quicker, like an engine that’s idling too fast. Naturally, this isn’t good for the engine.
Then there are the longer term implications of increased cortisol, with impacts on weight, sleep and memory.
At a time when many of us are struggling to make sense of what’s happening, and the events of pre-COVID seem a lifetime ago, it’s worth recognising how we’re built to respond to things like this, and what our brains do.
And one last thing.
Top and bottom
Typically, we have the capacity to manage how we’re feeling and the way we manage stress with our prefrontal cortex (PFC). This is the part of your brain just behind your forehead. It’s huge and complex and looks after what we call higher order tasks, or executive functions.
It’s role here is to help integrate our stress responses. It functions in a top down fashion, controlling what goes on. It’s complex and remarkable, but sensitive.
Stress also impacts working memory (what you’re using right now to ‘keep things in mind’) which is a PFC function. As stress continues, the PFC undergoes structural change. Its internal connections are weakened, and it just can’t function as it should.
Simultaneously, those same chemicals, the glucocorticoids and catecholamines, strengthen the emotional functions of your amygdala, your fear centre.
And so the scales tip.
Sustained stress flips how our brains control our behaviour, from top down to bottom up.
We lose the thoughtful, rational, reflective, top down ability of the PFC to control our behaviour. Instead, behaviour is controlled by the brutish, primitive, reflexive, bottom up amygdala.
Personal safety and threat avoidance are its goals. Refined thinking, reasoning, decision-making and deliberative thought, the preserve of the PFC, are lost.
Under the circumstances, maybe it isn’t entirely their fault.
Maybe we want to cut each other some slack.
Things are tough
Hopefully this is helpful in understanding why we might react or behave as we do in times of stress.
Extra notes
How to reduce cortisol and adrenaline
Simple, cost-effective ways to reduce cortisol and adrenaline
- A good sleep hygiene routine helps to get better sleep and reduce cortisol
- Limit caffeine, especially after lunch
- Get some exercise
- Nature (if you can get to it during lockdown) for a cumulative total of 2 hours a week
- Humour
- Social connection (electronic works too)
- Physical connection. Touch increases oxytocin, reducing cortisol.
- Blueberries and polyphenol-rich dark chocolate
- Relaxation, mindfulness, other stress management options
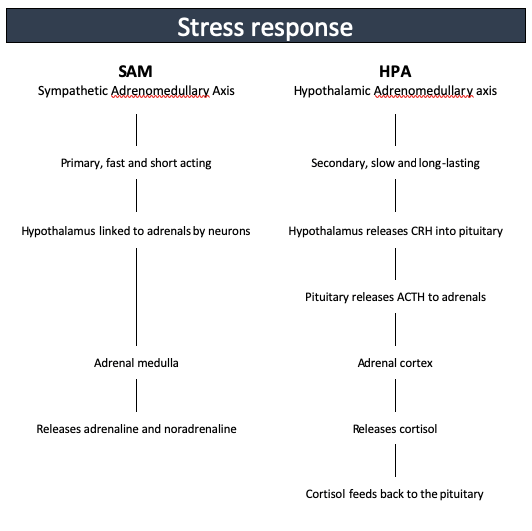
SAM/HPA summary

Pingback:When an employer wants you to 'build resilience' | Cerebra